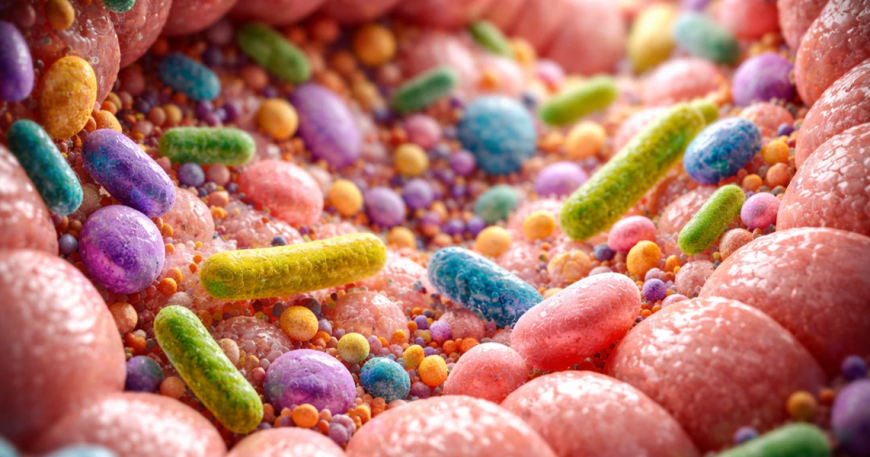
The human body is home to trillions of microorganisms, collectively known as the microbiome. Far from being passive passengers, these bacteria, viruses and fungi play a vital role in digestion, immune function and even mental health. In recent years, advances in sequencing technology and data analysis have transformed understanding of this complex ecosystem. The microbiome is now viewed not only as a marker of health, but as a potential target for innovative therapies.
As research accelerates, life sciences companies and academic institutions are exploring how manipulating the microbiome could prevent and treat disease.
Understanding the microbiome
The gut microbiome is the most studied microbial community in the body. It helps break down food, produce essential nutrients and protect against harmful pathogens. A balanced microbiome supports normal immune responses and metabolic function.
However, disruptions to this delicate ecosystem, often referred to as dysbiosis, have been linked to a range of conditions. These include inflammatory bowel disease, obesity, diabetes and certain autoimmune disorders. Emerging evidence also suggests a connection between the gut microbiome and mental health, through what is known as the gut-brain axis.
Understanding these relationships has opened new avenues for therapeutic intervention.
From probiotics to precision therapies
Early interest in the microbiome focused largely on probiotics and dietary supplements. While these products remain popular, scientific attention is increasingly shifting towards more targeted approaches.
Researchers are developing live biotherapeutic products, which contain specific strains of bacteria selected for their potential to treat particular conditions. Unlike general probiotics, these therapies are designed with defined mechanisms of action and undergo rigorous clinical testing.
Faecal microbiota transplantation, in which stool from a healthy donor is transferred to a patient, has already proven effective for recurrent Clostridioides difficile infection. Building on this success, scientists are investigating whether similar strategies could be adapted for other diseases.
Microbiome and personalised medicine
The composition of the microbiome varies significantly between individuals. Factors such as diet, environment, genetics and medication use all influence microbial balance. This variability aligns with the broader shift towards personalised medicine.
By analysing an individual’s microbiome profile, clinicians may one day tailor treatments more precisely. For example, understanding how a patient’s gut bacteria metabolise certain drugs could influence dosing decisions or predict side effects.
In oncology, researchers are examining how the microbiome affects responses to immunotherapy. Some studies suggest that specific bacterial populations may enhance or hinder the effectiveness of cancer treatments. If confirmed, modulating the microbiome could become part of standard care.
Challenges in translation
Despite growing enthusiasm, translating microbiome science into routine clinical practice presents challenges. The microbiome is extraordinarily complex, and cause-and-effect relationships are difficult to establish. Many associations observed in studies require further validation through large-scale trials.
Standardisation is another hurdle. Variations in sampling methods, sequencing techniques and data interpretation can lead to inconsistent findings. Establishing robust protocols will be essential to move from exploratory research to approved therapies.
Regulatory frameworks must also evolve. Live microbial therapies do not fit neatly into traditional categories of medicines, and ensuring safety and quality control requires careful oversight.
The UK’s role in microbiome research
The UK has emerged as a significant contributor to microbiome science. Academic institutions are conducting large-scale studies to map microbial diversity and explore its links to disease. Partnerships between universities, biotech firms and the NHS are supporting clinical trials of microbiome-based interventions.
National research funding and access to diverse patient populations provide a strong foundation for innovation. As understanding deepens, the UK is well positioned to translate discoveries into therapies that benefit patients domestically and internationally.
Looking ahead
The future of microbiome research is likely to extend beyond the gut. Scientists are exploring microbial communities in the skin, lungs and oral cavity, each with potential implications for health. Advances in artificial intelligence are helping to decode complex microbial interactions, accelerating discovery.
In time, routine healthcare may include microbiome profiling as part of preventative screening. Dietary advice, medication choices and targeted microbial therapies could be informed by an individual’s unique microbial signature.
Conclusion
The human microbiome represents one of the most intriguing frontiers in life sciences. Once overlooked, these microscopic communities are now recognised as central players in health and disease. By harnessing their therapeutic potential, researchers aim to develop more precise and effective treatments.
Significant scientific and regulatory challenges remain, but progress is steady. As evidence accumulates, microbiome-based therapies could become an integral component of personalised medicine. For patients and healthcare systems alike, understanding and modulating the microbiome offers a promising path towards improved outcomes and a more holistic view of health.